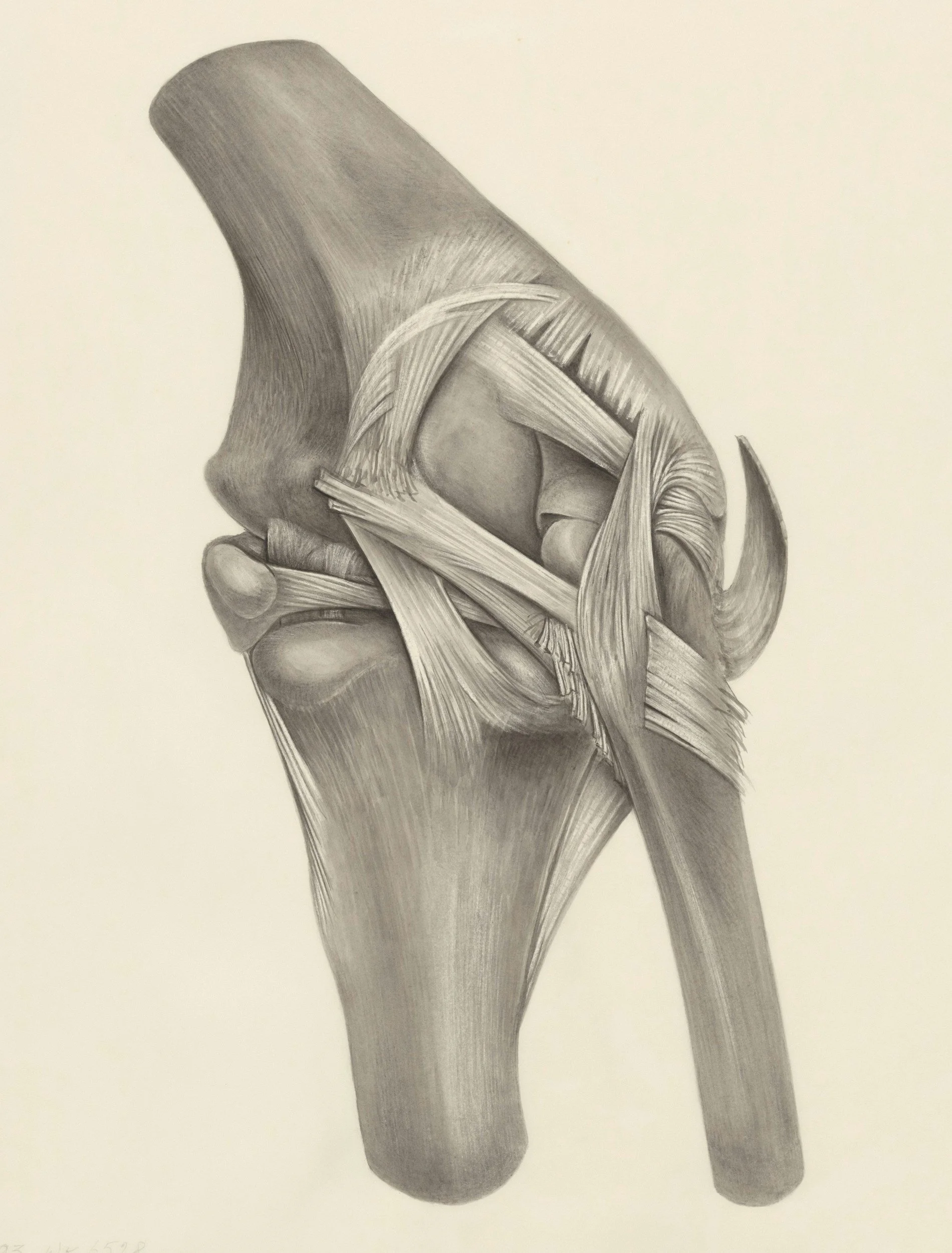
Spring Injury Surge: Why Activity Spikes Lead To More Pain And How To Prevent It
Spring consistently produces a predictable spike in musculoskeletal injuries. The primary driver is not the activity itself, but the rate of change in loading. During winter, overall movement volume drops—less walking, fewer sports, reduced variability in movement. This leads to decreased tendon stiffness, reduced neuromuscular coordination, and diminished joint stability. When activity resumes abruptly, tissues are exposed to forces they are no longer conditioned to tolerate.
Tendons are the limiting factor in this transition. Unlike muscle, which adapts relatively quickly, tendon remodeling occurs over weeks to months. This creates a false sense of readiness—patients feel capable, but their connective tissue is not. This mismatch commonly results in Achilles tendinopathy, patellar tendon irritation, and rotator cuff overload. Symptoms often appear with a delay (24–72 hours), leading patients to misattribute the cause.
Load progression must be deliberate. The widely accepted threshold is a 10–15% increase in weekly activity. Exceeding this significantly raises injury risk. Equally important is load distribution. Consecutive high-load days (e.g., running + gym + sports) create cumulative stress without adequate recovery windows. Tissue adaptation requires alternating stimulus and recovery.
Warm-up quality directly affects injury risk. Passive stretching alone does not prepare tissues for load. Activation-based warm-ups improve motor unit recruitment and joint stability. This reduces shear forces at joints and improves movement efficiency under load. Without proper activation, compensatory patterns dominate, increasing strain on vulnerable tissues.
Early symptom recognition determines outcome. Persistent stiffness, localized tendon pain, or asymmetry beyond several days indicates overload rather than simple soreness. Delaying intervention allows microdamage to accumulate into chronic pathology. Structured physiotherapy loading programs restore capacity and prevent long-term degeneration.
Practical Application (Physiotherapy-Based Exercises)
Glute Bridge (2–3 sets of 12)
Reinforces posterior chain activation to offload knees and lower backSingle-Leg Calf Raises (3 sets of 10–12 each side)
Progressive tendon loading for Achilles resilienceBanded Lateral Walks (2–3 sets of 15 steps)
Improves hip stability and reduces knee valgus stressDynamic Warm-Up (5–8 minutes)
Leg swings, walking lunges, arm circles, light jogging progressionWeekly Load Rule
Increase either duration OR intensity, never both simultaneously
References
Gabbett, T. J. (2016). Br J Sports Med, 50(5), 273–280.
Magnusson, S. P., & Kjaer, M. (2019). J Appl Physiol, 126(6), 1613–1621.
Kjaer, M., et al. (2009). Physiol Rev, 89(2), 537–578.
Bohm, S., et al. (2015). Sports Med, 45(5), 725–739.
Soligard, T., et al. (2016). Br J Sports Med, 50(9), 471–477.
Timmins, R. G., et al. (2016). Br J Sports Med, 50(24), 1529–1537.